Dizziness is the third most frequent complaint in general practice and the most common complaint in patients over 70 years of age. As many as 70% of adults 65 years and older complain of dizziness. Dizziness can describe many symptoms: vertigo, motion sensitivity, a sensation of movement, or a decrease in balance to name a few.
Just as there are many symptoms of dizziness, there are a multitude of causes for dizziness including inner ear weakness, decreased sensation, medications, canalith displacement, or other health problems. Several Bodies in Balance Physical Therapy employees have received specialty training to assess the causes of dizziness and to develop a customized plan to address the needs and to improve the condition of each individual.
The clinic has on-site diagnostic equipment such as Infrared Real-Eyes Goggles and the computerized Smart Balance Master system to assure accuracy in treatment planning. Therapist Karen Lambert, DPT, NCS has multiple publications with research regarding vestibular injuries and treatment. Our therapists treat patients with vestibular / dizziness disorders from as far as a 120-mile driving distance due to their recognized expertise in vestibular rehabilitation.
We have equipment and measures that have been proven to assess safety and function. We use these same measures to show improvements during the course of therapy.
Education is an important part of rehab to improve a person's condition, function and safety. There are some immediate ways to make your home safer and reduce your risk of falls.
- Benign Paroxysmal Positional Vertigo (BPPV)
- Migraine
- Cervicogenic (Neck Related) Vertigo
- Unilateral or Bilateral Hypofunction
- Central Vertigo or Balance Dysfunction
- Cardiac
- Medications
- Smart Balance Master
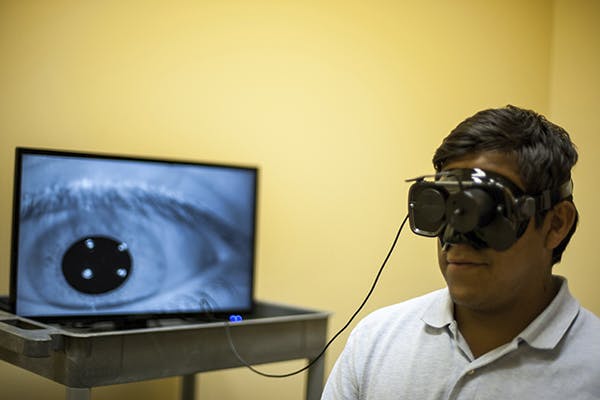
- Infrared Goggles
- Dynamic Visual Acuity Testing
- Maddox Rod Testing
- Balance and Exercises Equipment


Studies that show customized vestibular rehab has a greater benefit for patients who have dizziness than Tai Chi, strengthening, medication or a general physical therapy program.
Goals of Vestibular/Balance Rehab are to:- Decrease dizziness
- Improve mobility/activity/conditioning
- Increase safety, decrease risk of falls
- Increase head and trunk motion, including incorporating head motion during ambulation as well as quick turns while remaining stable and safe
- Decrease magnitude of symptoms
- Return to activities that provoke symptoms such as being in environments that stimulate problems with dizziness or balance including grocery store, malls, school, etc.

Falls can diminish your ability to lead an active and independent life. About one third of people over the age of 65 and almost half of people over the age of 80 will fall at least once this year. There usually are several reasons for a fall. Physical therapists can help you reduce your risk of falling by:
- Assessing your risk of falling
- Helping you make your home as safe as possible
- Educating you about the medical risk factors linked to falls
- Designing individualized exercises and balance training
- Working with other health care professionals and community services to create programs for people who want to reduce their risk of falling" APTA.org

Simple Steps to Reduce Fall Risks
- Improve balance and strength with exercise programs like Tai Chi, a Matter of Balance, and EnhanceFitness
- Reduce tripping hazards - keep cords, shoes, papers, plants, and boxes out of walkways
- Add grab bars in and beside the tub/shower and next to the toilet
- Use a nonslip mat or appliqués in the tub/shower
- Install railings on both sides of stairways
- Improve lighting and use night lights (motion sensor lights work well)
- Avoid throw rugs or use nonskid mats or tape
- Have your eyes checked by an eye doctor at least once a year
- Ask doctor or pharmacist to review your medications to identify those that may cause dizziness or drowsiness
Fall risk info from: https://www.cdc.gov/media/matte/2012/07_falls.pdf
How Your Balance System Works


Your sense of balance comes from many different systems working together to maintain the stability of your body and your vision. Good balance depends on correct information from several systems within your body, proper use of that information by your brain, and the right response from your muscles.
Sensory information comes to your brain from your visual, somatosensory, and vestibular systems:
Visual system: Your vision provides important information to the brain about your environment, such as where your body is in relation to the horizon while you're still or moving.
Somatosensory system: You have special sensors sensitive to stretch, pressure, vibration, and touch in your muscles, tendons, joints, and skin that help your brain to know how your body is positioned.
Vestibular system: Balance organs in your inner ear tell the brain about the movements and position of your head. This system senses your head movement and keeps your eyes focused. It also can tell the brain when your head is moving in a straight line (like when you're riding in a car or going up or down in an elevator) and also can sense the position of your head (upright or tilted) even when it is perfectly still.
The Brain's Role

Information from all of these systems travels to the brain stem. The brain stem also gets information from other parts of the brain, mostly about previous experiences that affect your sense of balance. Your brain can control balance by using the information that is most important for a particular situation. For instance:
In the dark, when the information from your eyes is reduced or might not be accurate, your brain will use more information from your legs and your inner ear.
If you are walking on a sandy beach during the day, the information coming from your legs and feet will be less reliable, and your brain will use information from your visual and vestibular systems more.
Once your brain stem sorts out all of this information, it sends messages to the eyes and other parts of your body to move in a way that will help you keep your balance and have clear vision while you are moving.


